Six Radical Visions for the Future of Health (including Self-Serve Pharma)
Today I gave the closing presentation at the National Medicine Symposium, rounding out deep discussion over several days on how to get better use of medicines. I developed six radical ideas that could be part of the future of health. The intention was to be provocative rather than rigorous, generating new ways of thinking about how healthcare may evolve.
Here are brief summaries of the six visions I presented:
1. Complete data.

Image source: Toto
The amount of information that we have about the health of an individual could become comprensive, generating terabytes of data from just one person. Bathrooms that monitor not just what we excrete but also analyze our skin color and tone as we look in the mirror are just the beginning. Images and sensors could record everything we eat and all medicines we take, providing far better analysis on the effectiveness of drugs. Odor is a highly data-intensive yet effective way to identify maladies. We could build virtually complete data sets of our health on a second by second basis.
2. Personalized medicine

In a world in which individual genomes can be sequenced, we can not only identify which drug will be most effective for the individual, but potentially also synthesize pharmaceuticals for one specific person. While the cost will be high, some will be prepared to pay and there will be pressure for insurers to bear the cost.
3. Radical life extension
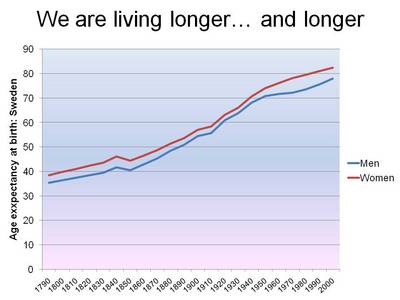
The trend for over two centuries is that for every decade that passes, life expectancy in developed countries increases by two years. If this varies, it is most likely to the upside, severely aggravating the existing aging of the population. The implications for healthcare would include not just new treatments, but a massive increase in aged care support.
4. Robot help
Robots and artificial intelligence will have manifold roles in healthcare, including avatar doctors, exoskeletons for nurses, and automated surgery. As I’ve written before, one of the most important tools will be emotional robots, that can demonstrate empathy and help patients in their recovery.
5. Modular R&D

The current pharmaceutical research and development chain is broken in many ways, driven by creating blockbuster drugs and rapidly running out of steam. There is an opportunity to break down R&D into discrete components from discovery through to clinical trials and regulatory approval, each of which is funded separately. If effective profit-share mechanisms can be created, risk will be distributed and there could be a flourishing of drugs developed for smaller markets. Innocentive, originally founded by Eli Lilly, is just the first step in distributed pharma innovation.
6. Self-serve pharma

Image credit: C-Ali
Patients now have massive medical information available, and they have the time and incentive to do research into what would be relevant to them. Why not throw out drug regulation, and leave people to make their own choices if they want? Most would rely on doctors, but others would self-medicate, usually extremely well. The world of self-serve pharma has already begun. How far will it go?
